Vol. 45 (5): 1080-1080, September – October, 2019
doi: 10.1590/S1677-5538.IBJU.2018.0495
VIDEO SECTION
Francesca Vedovo 1, Bernardino de Concilio 2, Guglielmo Zeccolini 2, Tommaso Silvestri 1, Antonio Celia 2
1 Department of Urology, Azienda Sanitaria Universitaria Integrata di Trieste, Trieste, Italy; 2 Department of Urology, San Bassiano Hospital, Bassano del Grappa, Italy
ABSTRACT
Introduction: Several techniques have been described to aid in the intra-operative identifi cation of the bladder diverticula.
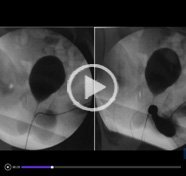
The video shows the peculiar advantage of using Firefl y Fluorescence Imaging da Vinci System® (FFIS) during bladder diverticula detection and dissection (BD).
Material and Methods: Patient is placed in the lithotomic position. A transperitoneal access to the bladder is preferred. A flexible cystoscopy with the FFIS is performed. This procedure facilitates the diverticulum detection. This near-infrared technology can be usefully utilized to facilitate the diverticulum dissection. Using sharp and blunt dissection, the diverticulum is totally resected. Bladder is sutured in two absorbable layers. Drainage is placed in the Retzius space and a peritoneum reconstruction is performed.
Results: Between 2016 and 2017, 4 BDs with intraoperative FFIS were performed in our Center. Median operative time was 110 minutes. Mean time of postoperative catheterization was 11 days and mean length of stay was 4 days. No significant post void residual neither urine extravasation after catheter removal occurred. No Clavien-Dindo post-operative complications ≥2 have been reported. Several approaches have been described for intra-operative diverticulum identification and its dissection: Parra used a cystoscopic transillumination of diverticulum; Das proposed the use of a Foley 50 mL balloon inserted in the diverticulum, while Nadler used a balloon catheter, placed in the diverticulum and bloated with 180 cc saline solution.
Conclusions: In our experience, intra-operative use of FFIS enhances the transillumination effect. The identification and dissection of the diverticulum is more rapid, safe and effective with no additional cost.
ARTICLE INFO
Available at: https://intbrazjurol.com.br/video-section/20180495_Vedovo_et_al